| SLC12A3 | |||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
 | |||||||||||||||||||||||||||||||||||||||||||||||||||
| Identifiers | |||||||||||||||||||||||||||||||||||||||||||||||||||
| Aliases | SLC12A3, NCC, NCCT, TSC, solute carrier family 12 member 3, Sodium-chloride symporter | ||||||||||||||||||||||||||||||||||||||||||||||||||
| External IDs | OMIM: 600968; MGI: 108114; HomoloGene: 287; GeneCards: SLC12A3; OMA: SLC12A3 - orthologs | ||||||||||||||||||||||||||||||||||||||||||||||||||
| |||||||||||||||||||||||||||||||||||||||||||||||||||
| |||||||||||||||||||||||||||||||||||||||||||||||||||
| |||||||||||||||||||||||||||||||||||||||||||||||||||
| |||||||||||||||||||||||||||||||||||||||||||||||||||
| |||||||||||||||||||||||||||||||||||||||||||||||||||
| Wikidata | |||||||||||||||||||||||||||||||||||||||||||||||||||
| |||||||||||||||||||||||||||||||||||||||||||||||||||
The sodium-chloride symporter (also known as Na+-Cl− cotransporter, NCC or NCCT, or as the thiazide-sensitive Na+-Cl− cotransporter or TSC) is a cotransporter in the kidney which has the function of reabsorbing sodium and chloride ions from the tubular fluid into the cells of the distal convoluted tubule of the nephron. It is a member of the SLC12 cotransporter family of electroneutral cation-coupled chloride cotransporters. In humans, it is encoded by the SLC12A3 gene (solute carrier family 12 member 3) located in 16q13. [5]
A loss of NCC function causes Gitelman syndrome, an autosomic recessive disease characterized by salt wasting and low blood pressure, hypokalemic metabolic alkalosis, hypomagnesemia and hypocalciuria. [6] Over a hundred different mutations in the NCC gene have been identified.
Molecular biology
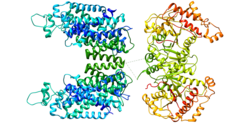
The sodium-chloride symporter or NCC is a member of the SLC12 cotransporter family of electroneutral cation-coupled chloride cotransporter, along with the potassium-chloride cotransporters (K+-Cl− cotransporters or KCCs), the sodium-potassium-chloride cotransporters (Na+-K+-Cl− cotransporters or NKCCs) and orphan member CIP ( cotransporter interacting protein) and CCC9. The sodium-chloride symporter's protein sequence has a high degree of identity between different mammalian species (over 90% between human, rat and mouse). The SLC12A3 gene encodes for a protein of 1,002 to 1,030 amino acid residues. NCC is a transmembrane protein, presumed to have a hydrophobic core of either 10 or 12 transmembrane domains with intracellular amino- and carboxyl-terminus domains. The exact structure of the NCC protein is unknown, as it has not yet been crystallized. The NCC protein forms homodimers at the plasma membrane.
N-glycosylation occurs in two sites in a long extracellular loop connecting two transmembrane domains within the hydrophobic core. This posttranslational modification is necessary for proper folding and transport of the protein to the plasma membrane. [7]
Function
Because NCC is located at the apical membrane of the distal convoluted tubule of the nephron, it faces the lumen of the tubule and is in contact with the tubular fluid. Using the sodium gradient across the apical membrane of the cells in distal convoluted tubule, the sodium-chloride symporter transports Na+ and Cl− from the tubular fluid into these cells. Afterward, the Na+ is pumped out of the cell and into the bloodstream by the Na+-K+ ATPase located at the basal membrane and the Cl− leaves the cells through the basolateral chloride channel ClC-Kb. The sodium-chloride symporter accounts for the absorption of 5% of the salt filtered at the glomerulus. NCC activity is known to have two control mechanisms affecting protein trafficking to the plasma membrane and transporter kinetics by phosphorylation and de-phosphorylation of conserved serine/threonine residues.
As NCC has to be at the plasma membrane to function, its activity can be regulated by increasing or decreasing the amount of protein at the plasma membrane. Some NCC modulators, such as the WNK3 and WNK4 kinases may regulate the amount of NCC at the cell surface by inducing the insertion or removal, respectively, of the protein from the plasma membrane. [8] [9]
Furthermore, many residues of NCC can be phosphorylated or dephosphorylated to activate or inhibit NCC uptake of Na+ and Cl−. Other NCC modulators, including intracellular chloride depletion, angiotensin II, aldosterone and vasopressin, can regulate NCC activity by phosphorylating conserved serine/threonine residues. [10] [11] [12] NCC activity can be inhibited by thiazides, which is why this symporter is also known as the thiazide-sensitive Na+-Cl− cotransporter. [5]
Pathology
Gitelman syndrome
A loss of NCC function is associated with Gitelman syndrome, an autosomic recessive disease characterized by salt wasting and low blood pressure, hypokalemic metabolic alkalosis, hypomagnesemia and hypocalciuria. [6]
Over a hundred different mutations in the NCC gene have been described as causing Gitelman syndrome, including nonsense, frameshift, splice site and missense mutations. Two different types of mutations exist within the group of missense mutations causing loss of NCC function. Type I mutations cause a complete loss of NCC function, in which the synthesized protein is not properly glycosylated. NCC protein harboring type I mutations is retained in the endoplasmic reticulum and cannot be trafficked to the cell surface. [13] Type II mutations cause a partial loss of NCC function in which the cotransporter is trafficked to the cell surface but has an impaired insertion in the plasma membrane. NCC harboring type II mutations have normal kinetic properties but are present in lower amounts at the cell surface, resulting in a decreased uptake of sodium and chloride. [14] NCC harboring type II mutations is still under control of its modulators and can still increase or decrease its activity in response to stimuli, whereas type I mutations cause a complete loss of function and regulation of the cotransporter. [15] However, in some patients with Gitelman's syndrome, no mutations in the NCC gene have been found despite extensive genetic work-up.
Hypertension and blood pressure
NCC has also been implicated to play a role in control of blood pressure in the open population, with both common polymorphisms and rare mutations altering NCC function, renal salt reabsorption and, presumably, blood pressure. Individuals with rare mutations in genes responsible for salt control in the kidney, including NCC, have been found to have a lower blood pressure than controls. [16] NCC harboring these mutations has a lower function than wild-type cotransporter although some mutations found in individuals in the open population seem to be less deleterious to cotransporter function than mutations in individuals with Gitelman's syndrome. [15]
Furthermore, heterozygous carriers of mutations causing Gitelman syndrome (i.e. individuals who have a mutation in one of the two alleles and do not have the disease) have a lower blood pressure than non-carriers in the same family. [17]
Pseudohypoaldosteronism type II
Type II pseudohypoaldosteronism (PHA2), also known as Gordon's syndrome, is an autosomal dominant disease in which there is an increase in NCC activity leading to short stature, increased blood pressure, increased serum K+ levels, increased urinary calcium excretion and hyperchloremic metabolic acidosis. However, PHA2 is not caused by mutations within the NCC gene, but by mutations in NCC regulators WNK1 and WNK4. Patients respond well to treatment with thiazide-type diuretics.
See also
- Nephron
- Distal convoluted tubule
- Electrolytes, such as sodium and chloride
- Cotransporter, including symporter
- Blood pressure
- Diuretics and thiazides
References
- ^ a b c GRCh38: Ensembl release 89: ENSG00000070915 – Ensembl, May 2017
- ^ a b c GRCm38: Ensembl release 89: ENSMUSG00000031766 – Ensembl, May 2017
- ^ "Human PubMed Reference:". National Center for Biotechnology Information, U.S. National Library of Medicine.
- ^ "Mouse PubMed Reference:". National Center for Biotechnology Information, U.S. National Library of Medicine.
- ^ a b Mastroianni N, De Fusco M, Zollo M, Arrigo G, Zuffardi O, Bettinelli A, Ballabio A, Casari G (August 1996). "Molecular cloning, expression pattern, and chromosomal localization of the human Na-Cl thiazide-sensitive cotransporter (SLC12A3)". Genomics. 35 (3): 486–93. doi: 10.1006/geno.1996.0388. PMID 8812482.
- ^ a b Knoers NV, Levtchenko EN (2008). "Gitelman syndrome". Orphanet J Rare Dis. 3: 22. doi: 10.1186/1750-1172-3-22. PMC 2518128. PMID 18667063.
- ^ Gamba G (May 2009). "The thiazide-sensitive Na+-Cl− cotransporter: molecular biology, functional properties, and regulation by WNKs". American Journal of Physiology. Renal Physiology. 297 (4): F838–48. doi: 10.1152/ajprenal.00159.2009. PMC 3350128. PMID 19474192.
- ^ Rinehart J, Kahle K, de los Heros P, Vazquez N, Meade P, Wilson F, Hebert S, Gimenez I, Gamba G, Lifton R (November 2005). "WNK3 kinase is a positive regulator of NKCC2 and NCC, renal cation-Cl− cotransporters required for normal blood pressure homeostasis". PNAS. 102 (46): 16777–16782. Bibcode: 2005PNAS..10216777R. doi: 10.1073/pnas.0508303102. PMC 1283841. PMID 16275913.
- ^ Zhou B, Zhuang J, Gu D, Wang H, Cebotaru L, Guggino W, Cai H (January 2010). "WNK4 Enhances the Degradation of NCC through a Sortilin-Mediated Lysosomal Pathway". Journal of the American Society of Nephrology. 21 (1): 82–92. doi: 10.1681/ASN.2008121275. PMC 2799281. PMID 19875813.
- ^ Pacheco-Alvarez D, San Cristóbal P, Meade P, Moreno E, Vazquez N, Muñoz E, Díaz A, Juárez ME, Giménez I, Gamba G (August 2006). "The Na+:Cl− Cotransporter Is Activated and Phosphorylated at the Amino-terminal Domain upon Intracellular Chloride Depletion". J. Biol. Chem. 281 (39): 28755–28763. doi: 10.1074/jbc.M603773200. PMID 16887815.
- ^ van der Lubbe N, Lim C, Fenton R, Meima M, Jan Danser A, Zietse R, Hoorn E (August 2010). "Angiotensin II induces phosphorylation of the thiazide-sensitive sodium chloride cotransporter independent of aldosterone". Kidney International. 79 (1): 66–76. doi: 10.1038/ki.2010.290. PMID 20720527.
- ^ Pedersen NB, Hofmeister MV, Rosenbaek LL, Nielsen J, Fenton RA (July 2010). "Vasopressin induces phosphorylation of the thiazide-sensitive sodium chloride cotransporter in the distal convoluted tubule". Kidney International. 78 (2): 160–169. doi: 10.1038/ki.2010.130. PMID 20445498.
- ^ de Jong JC, can der Vliet WA, van den Heuvel LPWJ, Willems PHGM, Knoers NVAM, Bindels RJM (2002). "Functional Expression of Mutations in the Human NaCl Cotransporter: Evidence for Impaired Routing Mechanisms in Gitelman's Syndrome". Journal of the American Society of Nephrology. 13 (6): 1442–1448. doi: 10.1097/01.ASN.0000017904.77985.03. PMID 12039972.
- ^ Sabath E, Meade P, Berkman J, de los Heros P, Moreno E, Bobadilla NA, Vázquez N, Ellison DH, Gamba G (2004). "Pathophysiology of functional mutations of the thiazide-sensitive Na-Cl cotransporter in Gitelman disease". Am J Physiol Renal Physiol. 287 (2): F195–F203. doi: 10.1152/ajprenal.00044.2004. PMID 15068971.
- ^ a b Acuña R, Martínez de la Maza L, Ponce-Coria J, Vázquez N, Ortal-Vite P, Pacheco-Alvarez D, Bobadilla NA, Gamba G (2009). "Rare mutations in SLC12A1 and SLC12A3 protect against hypertension by reducing the activity of renal salt cotransporters". Journal of Hypertension. 29 (3): 475–83. doi: 10.1097/HJH.0b013e328341d0fd. PMID 21157372. S2CID 205630437.
- ^ Weizhen Ji, Jia Nee Foo, Brian J O'Roak, Hongyu Zhao, Martin G Larson, David B Simon, Christopher Newton-Cheh, Matthew W State, Daniel Levy, Richard P Lifton (2008). "Rare independent mutations in renal salt handling genes contribute to blood pressure variation". Nature Genetics. 40 (5): 592–599. doi: 10.1038/ng.118. PMC 3766631. PMID 18391953.
- ^ Fava C, Montagnana M, Rosberg L, Burri P, Almgren P, Jönsson A, Wanby P, Lippi G, Minuz P, Hulthèn G, Aurell M, Melander O (2008). "Subjects heterozygous for genetic loss of function of the thiazide-sensitive cotransporter have reduced blood pressure". Hum. Mol. Genet. 17 (3): 413–18. doi: 10.1093/hmg/ddm318. PMID 17981812.
Further reading
- Kamdem LK, Hamilton L, Cheng C, et al. (2008). "Genetic predictors of glucocorticoid-induced hypertension in children with acute lymphoblastic leukemia". Pharmacogenet. Genomics. 18 (6): 507–14. doi: 10.1097/FPC.0b013e3282fc5801. PMID 18496130. S2CID 1251203.
- Coto E, Arriba G, GarcÃa-Castro M, et al. (2009). "Clinical and analytical findings in Gitelman's syndrome associated with homozygosity for the c.1925 G>A SLC12A3 mutation". Am. J. Nephrol. 30 (3): 218–21. doi: 10.1159/000218104. PMID 19420906. S2CID 41050205.
- Yasujima M, Tsutaya S (2009). "[Mutational analysis of a thiazide-sensitive Na-Cl cotransporter (SLC12A3) gene in a Japanese population—the Iwaki Health Promotion Project]". Rinsho Byori. 57 (4): 391–6. PMID 19489442.
- Shao L, Liu L, Miao Z, et al. (2008). "A novel SLC12A3 splicing mutation skipping of two exons and preliminary screening for alternative splice variants in human kidney". Am. J. Nephrol. 28 (6): 900–7. doi: 10.1159/000141932. PMID 18580052. S2CID 19321638.
- van Rijn-Bikker PC, Mairuhu G, van Montfrans GA, et al. (2009). "Genetic factors are relevant and independent determinants of antihypertensive drug effects in a multiracial population". Am. J. Hypertens. 22 (12): 1295–302. doi: 10.1038/ajh.2009.192. PMID 19779464.
- Shao L, Ren H, Wang W, et al. (2008). "Novel SLC12A3 mutations in Chinese patients with Gitelman's syndrome". Nephron Physiol. 108 (3): 29–36. doi: 10.1159/000117815. PMID 18287808. S2CID 25283004.
- Ji W, Foo JN, O'Roak BJ, et al. (2008). "Rare independent mutations in renal salt handling genes contribute to blood pressure variation". Nat. Genet. 40 (5): 592–9. doi: 10.1038/ng.118. PMC 3766631. PMID 18391953.
- Riveira-Munoz E, Devuyst O, Belge H, et al. (2008). "Evaluating PVALB as a candidate gene for SLC12A3-negative cases of Gitelman's syndrome". Nephrol. Dial. Transplant. 23 (10): 3120–5. doi: 10.1093/ndt/gfn229. PMID 18469313.
- Zhou B, Zhuang J, Gu D, et al. (2010). "WNK4 enhances the degradation of NCC through a sortilin-mediated lysosomal pathway". J. Am. Soc. Nephrol. 21 (1): 82–92. doi: 10.1681/ASN.2008121275. PMC 2799281. PMID 19875813.
- Hsu YJ, Yang SS, Chu NF, et al. (2009). "Heterozygous mutations of the sodium chloride cotransporter in Chinese children: prevalence and association with blood pressure". Nephrol. Dial. Transplant. 24 (4): 1170–5. doi: 10.1093/ndt/gfn619. PMID 19033254.
- Nozu K, Iijima K, Nozu Y, et al. (2009). "A deep intronic mutation in the SLC12A3 gene leads to Gitelman syndrome". Pediatr. Res. 66 (5): 590–3. doi: 10.1203/PDR.0b013e3181b9b4d3. PMID 19668106.
- Ng DP, Nurbaya S, Choo S, et al. (2008). "Genetic variation at the SLC12A3 locus is unlikely to explain risk for advanced diabetic nephropathy in Caucasians with type 2 diabetes". Nephrol. Dial. Transplant. 23 (7): 2260–4. doi: 10.1093/ndt/gfm946. PMID 18263927.
- Aoi N, Nakayama T, Sato N, et al. (2008). "Case-control study of the role of the Gitelman's syndrome gene in essential hypertension". Endocr. J. 55 (2): 305–10. doi: 10.1507/endocrj.K07E-021. PMID 18362449.
- Qin L, Shao L, Ren H, et al. (2009). "Identification of five novel variants in the thiazide-sensitive NaCl co-transporter gene in Chinese patients with Gitelman syndrome". Nephrology (Carlton). 14 (1): 52–8. doi: 10.1111/j.1440-1797.2008.01042.x. PMID 19207868. S2CID 38008467.
- Ridker PM, Paré G, Parker AN, et al. (2009). "Polymorphism in the CETP gene region, HDL cholesterol, and risk of future myocardial infarction: Genomewide analysis among 18 245 initially healthy women from the Women's Genome Health Study". Circ Cardiovasc Genet. 2 (1): 26–33. doi: 10.1161/CIRCGENETICS.108.817304. PMC 2729193. PMID 20031564.
- Richardson C, Rafiqi FH, Karlsson HK, et al. (2008). "Activation of the thiazide-sensitive Na+-Cl− cotransporter by the WNK-regulated kinases SPAK and OSR1". J. Cell Sci. 121 (Pt 5): 675–84. doi: 10.1242/jcs.025312. PMID 18270262. S2CID 33009059.
- Wang XF, Lin RY, Wang SZ, et al. (2008). "Association study of variants in two ion-channel genes (TSC and CLCNKB) and hypertension in two ethnic groups in Northwest China". Clin. Chim. Acta. 388 (1–2): 95–8. doi: 10.1016/j.cca.2007.10.017. PMID 17997379.
- Miao Z, Gao Y, Bindels RJ, et al. (2009). "Coexistence of normotensive primary aldosteronism in two patients with Gitelman's syndrome and novel thiazide-sensitive Na–Cl cotransporter mutations". Eur. J. Endocrinol. 161 (2): 275–83. doi: 10.1530/EJE-09-0271. hdl: 2066/80977. PMID 19451210.
- Zhan YY, Jiang X, Lin G, et al. (2007). "[Association of thiazide-sensitive Na+-Cl* cotransporter gene polymorphisms with the risk of essential hypertension]". Zhonghua Yi Xue Yi Chuan Xue Za Zhi. 24 (6): 703–5. PMID 18067089.
External links
- Sodium+Chloride+Symporters at the U.S. National Library of Medicine Medical Subject Headings (MeSH)
- Sodium+Chloride+Symporter+Inhibitors at the U.S. National Library of Medicine Medical Subject Headings (MeSH)