| Low-level laser therapy | |
|---|---|
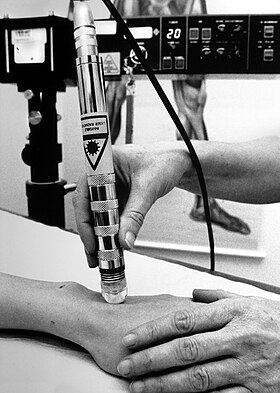 LLLT being applied for rheumatism in Sweden | |
| MeSH | D028022 |
Low-level laser therapy (LLLT), cold laser therapy, photobiomodulation (PBM) [1] [2] [3] [4] or red light therapy [5] is a form of medicine that applies low-level (low- power) lasers or light-emitting diodes (LEDs) to the surface of the body. Whereas high-power lasers are used in laser medicine to cut or destroy tissue, it is claimed that application of low-power lasers relieves pain or stimulates and enhances cell function. The effects appear to be limited to a specified set of wavelengths and new research has demonstrated effectiveness at myopia control. [6] Several such devices are cleared by the United States Food and Drug Administration (FDA), and research shows potential for treating a range of medical problems including rheumatoid arthritis [7] and oral mucositis. [8]
Mechanism
|
| This section needs expansion. You can help by
adding to it. (June 2023) |
Research is ongoing about the mechanism of LLLT. The effects of LLLT appear to be limited to a specified set of wavelengths of laser, [9] and administering LLLT below the dose range does not appear to be effective. [10] Photochemical reactions are well known in biological research, and LLLT make use of the first law in photochemistry ( Grotthuss-Draper law): light must be absorbed by a chemical substance in order for a photochemical reaction to take place. In LLLT that chemical substance is represented by the respiratory enzyme cytochrome c oxidase which is involved in the electron transport chain in mitochondria, [11] [12] which is the generally accepted theory.
Medical uses
Various LLLT devices have been promoted for use in treatment of several musculoskeletal conditions including carpal tunnel syndrome (CTS), fibromyalgia, osteoarthritis, and rheumatoid arthritis. They have also been promoted for temporomandibular joint disorders, wound healing, smoking cessation, and tuberculosis. LLLT appears to be effective for preventing oral mucositis in recipients of a stem cell transplant with chemotherapy. [8] [13] In other areas, evidence for LLLT remains conflicted. Some studies suggest that LLLT may be modestly effective in relieving short-term pain for rheumatoid arthritis, [7] osteoarthritis, [14] chronic low back pain, [15] acute and chronic neck pain, [16] tendinopathy, [9] [17] and chronic joint disorders. [10] The evidence for LLLT being useful in dentistry, [18] [19] and in the treatment of wound healing [20] is unclear.
Veterinary use
Veterinary clinics use cold laser devices to treat a wide variety of ailments, from arthritis to wounds, on dogs and cats. [21] [22] Very little research has been done on the effects of this treatment on animals. Brennen McKenzie, president of the Evidence-Based Veterinary Medicine Association, has stated that "research into cold laser in dogs and cats is sparse and generally low quality. Most studies are small and have minimal or uncertain controls for bias and error". [23] [24] While allowing that some studies show promising results, he reports that others do not. While believing that there is enough evidence to warrant further study, he concludes that there is not enough evidence to support routine clinical use of cold laser in animals.
Society and culture
History
Faroese physician Niels Finsen is believed to be the father of modern light therapy. [25] He used red light to treat smallpox lesions. He received the Nobel Prize in Physiology or Medicine in 1903. [26] Scientific evidence for some of his treatments is lacking, and later eradication of smallpox and development of antibiotics for tuberculosis rendered light therapy obsolete for these diseases. [27]
Hungarian physician and surgeon Endre Mester (1903–1984) is credited with the discovery of the biological effects of low power lasers, [28] which occurred a few years after the 1960 invention of the ruby laser and the 1961 invention of the helium–neon (HeNe) laser. [11] Mester accidentally discovered that low-level ruby laser light could regrow hair during an attempt to replicate an experiment that showed that such lasers could reduce tumors in mice. The laser he was using was faulty and wasn't as powerful as he thought. It failed to affect the tumors, but he noticed that in the places where he had shaved the mice in order to do the experiments, the hair grew back more quickly on the treated mice than on those among the control group. [2] He published those results in 1967. [11] He went on to show that low level HeNe light could accelerate wound healing in mice. [11]
By the 1970s, he was applying low level laser light to treat people with skin ulcers. [11] In 1974, he founded the Laser Research Center at the Semmelweis Medical University in Budapest, and continued working there for the remainder of his life. [29] His sons carried on his work and brought it to the United States. [28] By 1987, companies selling lasers were claiming that they could treat pain, accelerate healing of sports injuries, and treat arthritis, but there was little evidence for this at that time. [28] Mester originally called this approach "laser biostimulation'", but it soon became known as “low-level laser therapy" and with the adaptation of light emitting diodes by those studying this approach, it became known as "low-level light therapy", and to resolve confusion around the exact meaning of "low level", the term "photobiomodulation" arose. [2]
Names
The following terms are accepted as alternatives of low level light therapy term: LLLT, laser biostimulation, laser phototherapy, low-level laser therapy, low-power laser irradiation, low-power laser therapy, and photobiomodulation therapy. The term photobiomodulation therapy is considered the preferred term by industry professionals. [3] [4] However LLLT has been marketed and researched under a number of other terms, including red light therapy, [30] low-power laser therapy (LPLT), soft laser therapy, low-intensity laser therapy, low-energy laser therapy, cold laser therapy, bio-stimulation laser therapy, photo-biotherapy, therapeutic laser, and monochromatic infrared light energy (MIRE) therapy. [31] More specific applications sometimes have their own terms, for example when administered to acupuncture points, the procedure is called laser acupuncture. When applied to the head, LLLT may be known as transcranial photobiomodulation, transcranial near-infrared laser therapy (NILT), [32] or transcranial low level light therapy.
Government action
The FDA filed a complaint for injunction in 2014, alleging that company QLaser PMA were marketing their devices as being able to treat “over 200 different diseases and disorders,” including cancer, cardiac arrest, deafness, diabetes, HIV/AIDS, macular degeneration, and venereal disease. This case resulted in a permanent injunction against the manufacture, marketing, sale, and distribution of those devices in 2015. [33]
In 2017, the owner of QLaser, Robert Lytle, and two of QLaser's distributors were charged with a criminal conspiracy to commit fraud. Lytle pleaded guilty to one count of conspiracy to introduce misbranded medical devices into interstate commerce with the intent to defraud and mislead, and one count of criminal contempt in January 2018. Lytle was sentenced to serve 12 years in prison and made an initial restitution payment of $637,000. Lytle's conspirators were sentenced to 24 months and 15 months, respectively. [34] [35]
Reimbursement
The examples and perspective in this section may not represent a
worldwide view of the subject. (January 2024) |
Blue Cross Blue Shield Association and Aetna provide coverage for the prevention of oral mucositis, but not any other reason. [36] [37] The Centers for Medicare and Medicaid Services does not provide coverage for LLLT. [38] Cigna lists LLLT as "experimental, investigational, or unproven for any indication" and provides literature review summaries for a number of conditions. [39]
Research

Musculoskeletal
Evidence does not support a benefit in delayed-onset muscle soreness. [40] It may be useful for muscle pain and injuries. [41] A 2008 Cochrane Library review concluded that LLLT has insufficient evidence for treatment of nonspecific low back pain, [42] a finding echoed in a 2010 review of chronic low back pain. [43] A 2015 review found benefit in nonspecific chronic low-back pain. [15] LLLT may be useful in the treatment of both acute and chronic neck pain. [16] In 2013, however, a systematic review and meta-analysis of LLLT for neck pain indicated that the benefit was not of significant importance and that the evidence had a high risk of bias. [44] In a study testing the efficacy of low-level laser therapy treating plantar fasciitis found that LLLT significantly reduces pain in lower extremity tendinopathy and plantar fasciitis in the short and medium terms. [45] The same study also stated that while comparing the effect of LLLT to that of therapeutic ultrasound in persons with patellar tendinopathy, and they found a statistically significant effect in favour of LLLT, both on pain reduction and function. [46]
There are tentative data that LLLT is useful in the short-term treatment of pain caused by rheumatoid arthritis, [7] and possibly chronic joint disorders. [10] Research that compared the effects of LLLT against other treatments, sham treatments, or no treatment at all, and randomized adult patients with rheumatoid arthritis to receive it were considered. These outcomes included pain, functional capacity, adverse events, inflammation, disease activity, range of motion, stiffness in the morning, muscle strength, and quality of life. [47] The findings indicate that the differences between utilizing a sham and an infrared laser may be negligible or nonexistent in terms of pain, stiffness in the morning, grip strength, functional ability, inflammation, range of motion, disease activity, and side events. We also discovered that the data about the effects of laser acupuncture against reflexology in terms of functional ability, quality of life, and inflammation is quite hazy, and about the effects of red laser versus sham in terms of pain, morning stiffness, and side events. [48] The usefulness of red laser, laser acupuncture, and reflexology in the treatment of RA patients is not well enough demonstrated. [49] A 2019 systematic review and meta-analysis found evidence for pain reduction in osteoarthritis. [14] While it does not appear to improve pain in temporomandibular disorders, it may improve function. [50]
There is tentative evidence of benefit in tendinopathy. [9] [17] A 2014 review found benefit in shoulder tendinopathy. [51] A 2014 Cochrane review found tentative evidence that it may help in frozen shoulders. [52]
Mouth
Similarly, the use of lasers to treat chronic periodontitis [18] and to speed healing of infections around dental implants [19] is suggested, but there is insufficient evidence to indicate a use superior to traditional practices. [53] There is tentative evidence for dentin hypersensitivity. [54] It does not appear to be useful for orthodontic pain [55] [56] LLLT might be useful for wisdom tooth extraction (complications). [57]
Hair loss
LLLT has been studied as a treatment for hair loss; a review in 2012 found little evidence to support the use of lasers to treat hair loss. [58] A 2014 review found tentative evidence for benefit for lasers, [59] while another 2014 review concluded that the results were mixed, had a high risk of bias, and that its effectiveness was unclear. [60] A 2015 review found tentative evidence of benefit. [61] Additionally, a 2017 review of clinical trials found 10 of 11 trials reviewed "demonstrated significant improvement of androgenic alopecia in comparison to baseline or controls when treated with LLLT." [62]
LLLT is shown to increase hair density and growth in both genders. The types of devices (hat, comb, helmet) and duration did not alter the effectiveness, [63] with more emphasis to be placed on lasers compared to LEDs. [64] Ultraviolet and infrared light are more effective for alopecia areata, while red light and infrared light is more effective for androgenetic alopecia. [65]
Medical reviews suggest that LLLT is as effective or potentially more than other non invasive and traditional therapies like minoxidil and finasteride but further studies such as RCTs, long term follow up studies, and larger double blinded trials need to be conducted to confirm the initial findings. [66] [67] [68]
Brain injuries
LLLT has been studied for traumatic brain injury (TBI) and stroke among other conditions. [11] When applied to the head it is known as transcranial photobiomodulation or transcranial low level light therapy.
Cancer treatment side effects
LLLT has been studied as a way to reduce pain and swelling in breast-cancer related lymphedema. [69] [20] The 2015 systematic review & meta-analysis by Smoot, Chiavola-Larson, et al found: “Moderate-strength evidence supports LLLT in the management of [breast cancer related lymphoedema], with […] reductions in volume and pain immediately after conclusion of LLLT treatments. Greater reductions in volume [of lymph nodes or surrounding tissues] were found with the use of LLLT than in treatments without it.” [70]
Stem cells
An ongoing area of research is the application of LLLT for increasing cell proliferation, including stem cells. [71]
Wound healing
Low level laser therapy has been studied as a potential treatment for chronic wounds, and higher-power lasers have sometimes been successfully used to close acute wounds as an alternative to stitching. [72] However, as of 2012 [update] and due to inconsistent results and the low quality of extant research, reviews in the scientific literature have not supported its widespread application. [72] [73]
See also
References
- ^ Hamblin MR (2016). "Photobiomodulation or low-level laser therapy". Journal of Biophotonics. 9 (11–12): 1122–1124. doi: 10.1002/jbio.201670113. PMC 5215795. PMID 27973730.
- ^ a b c Hamblin MR (1 October 2016). "Shining light on the head: Photobiomodulation for brain disorders". BBA Clinical. 6: 113–124. doi: 10.1016/j.bbacli.2016.09.002. PMC 5066074. PMID 27752476.
- ^ a b Hamblin MR, Carroll JD, de Freitas LF, Huang YY, Ferraresi C (2018-01-12), "Introduction", Low-Level Light Therapy: Photobiomodulation, SPIE, doi: 10.1117/3.2295638.ch1, ISBN 978-1-5106-1416-1, retrieved 2021-02-11
- ^ a b "Photobiomodulation". www.aslms.org. Retrieved 2019-09-02.
- ^ Hamblin MR, Gupta A (2013). "History and Fundamentals of Low-Level Laser (Light) Therapy". In Hamblin MR, Huang Y (eds.). Handbook of Photomedicine. CRC Press. doi: 10.1201/b15582-10. ISBN 978-0-429-19384-2. Retrieved 2023-09-04.
- ^ Jiang Y, Zhuoting Z, Xingping T, Xiangbin K, Zhong H, Zhang J, Xiong R, Yuan Y, Zeng J (2021-12-01). "Effect of Repeated Low-Level Red-Light Therapy for Myopia Control in Children". American Academy of Ophthalmology.
- ^ a b c Brosseau L, Welch V, Wells GA, de Bie R, Gam A, Harman K, Morin M, Shea B, Tugwell P (2005). "Low level laser therapy (Classes I, II and III) for treating rheumatoid arthritis". Cochrane Database of Systematic Reviews. 2010 (4): CD002049. doi: 10.1002/14651858.CD002049.pub2. PMC 8406947. PMID 16235295. S2CID 40986179.
- ^ a b Oberoi S, Zamperlini-Netto G, Beyene J, Treister NS, Sung L (2014). "Effect of prophylactic low level laser therapy on oral mucositis: a systematic review and meta-analysis". PLOS ONE. 9 (9): e107418. Bibcode: 2014PLoSO...9j7418O. doi: 10.1371/journal.pone.0107418. PMC 4157876. PMID 25198431.
- ^ a b c Bjordal JM, Lopes-Martins RA, Joensen J., Couppe C., Ljunggren AE, Stergioulas A., Johnson MI (2008). "A systematic review with procedural assessments and meta-analysis of Low Level Laser Therapy in lateral elbow tendinopathy (tennis elbow)". BMC Musculoskeletal Disorders. 9: 75. doi: 10.1186/1471-2474-9-75. PMC 2442599. PMID 18510742.
- ^ a b c Bjordal JM, Couppé C, Chow RT, Tunér J, Ljunggren EA (2003). "A systematic review of low level laser therapy with location-specific doses for pain from chronic joint disorders". The Australian Journal of Physiotherapy. 49 (2): 107–16. doi: 10.1016/s0004-9514(14)60127-6. PMID 12775206.
- ^ a b c d e f Chung H, Dai T, Sharma SK, Huang YY, Carroll JD, Hamblin MR (2011). "The Nuts and Bolts of Low-level Laser (Light) Therapy". Annals of Biomedical Engineering. 40 (2): 516–533. doi: 10.1007/s10439-011-0454-7. ISSN 0090-6964. PMC 3288797. PMID 22045511.
- ^ Prindeze NJ, Moffatt LT, Shupp JW (2012-11-01). "Mechanisms of action for light therapy: a review of molecular interactions". Experimental Biology and Medicine. 237 (11): 1241–1248. doi: 10.1258/ebm.2012.012180. ISSN 1535-3699. PMID 23239434. S2CID 227103.
- ^ On behalf of The Mucositis Study Group of the Multinational Association of Supportive Care in Cancer/International Society of Oral Oncology (MASCC/ISOO), Zadik Y, Arany PR, Fregnani ER, Bossi P, Antunes HS, Bensadoun RJ, Gueiros LA, Majorana A (October 2019). "Systematic review of photobiomodulation for the management of oral mucositis in cancer patients and clinical practice guidelines". Supportive Care in Cancer. 27 (10): 3969–3983. doi: 10.1007/s00520-019-04890-2. hdl: 11379/522893. ISSN 0941-4355. PMID 31286228.
- ^ a b Stausholm MB, Naterstad IF, Joensen J, Lopes-Martins RÁ, Sæbø H, Lund H, Fersum KV, Bjordal JM (2019-10-28). "Efficacy of low-level laser therapy on pain and disability in knee osteoarthritis: systematic review and meta-analysis of randomised placebo-controlled trials". BMJ Open. 9 (10): e031142. doi: 10.1136/bmjopen-2019-031142. ISSN 2044-6055. PMC 6830679. PMID 31662383.
- ^
a
b Huang Z, Ma J, Chen J, Shen B, Pei F, Kraus VB (2015-12-15).
"The effectiveness of low-level laser therapy for nonspecific chronic low back pain: a systematic review and meta-analysis". Arthritis Research & Therapy. 17: 360.
doi:
10.1186/s13075-015-0882-0 (inactive 2024-02-27).
ISSN
1478-6362.
PMC
4704537.
PMID
26667480.
{{ cite journal}}: CS1 maint: DOI inactive as of February 2024 ( link) - ^ a b Chow R, Johnson M, Lopes-Martins R, Bjordal J (Nov 2009). "Efficacy of low-level laser therapy in the management of neck pain: a systematic review and meta-analysis of randomised placebo or active-treatment controlled trials". Lancet. 374 (9705): 1897–1908. doi: 10.1016/S0140-6736(09)61522-1. PMID 19913903. S2CID 16336402.
- ^ a b Tumilty S., Munn J., McDonough S., Hurley DA, Basford JR, Baxter GD (2010). "Low Level Laser Treatment of Tendinopathy: A Systematic Review with Meta-analysis". Photomedicine and Laser Surgery. 28 (1): 3–16. doi: 10.1089/pho.2008.2470. PMID 19708800. S2CID 10634480.
- ^ a b Cobb CM (2006). "Lasers in Periodontics: A Review of the Literature". Journal of Periodontology. 77 (4): 545–564. doi: 10.1902/jop.2006.050417. PMID 16584335. S2CID 16452438.
- ^ a b Sculean A, Schwarz F, Becker J (2005). "Anti-infective therapy with an Er:YAG laser: influence on peri-implant healing". Expert Review of Medical Devices. 2 (3): 267–76. doi: 10.1586/17434440.2.3.267. PMID 16288590. S2CID 5544626.
- ^ a b Da Silva JP, Da Silva MA, Almeida AP, Junior IL, Matos AP (2010). "Laser Therapy in the Tissue Repair Process: A Literature Review". Photomedicine and Laser Surgery. 28 (1): 17–21. doi: 10.1089/pho.2008.2372. PMID 19764898.
- ^ "Doggone Joints: Laser Therapy for Pet Arthritis". ABC News. 2011-02-23. Retrieved 2016-07-19.
- ^ Robinson, Narda G. (2013), "Complementary and Alternative Veterinary Medicine: Laser Therapy", The Merck Veterinary Manual, 11th edition.
- ^ McKenzie, Brennen (2016), "The Laser Craze: What Is the Evidence for Low-level Laser Therapy?" Archived 2018-01-10 at the Wayback Machine [SA222]; Western Veterinary Conference, Proceedings of the WVC 88th Annual Conference, Mandalay Bay Convention Center, Resort and Casino, Las Vegas, NV, March 6–10, 2016.
- ^ McKenzie, Brennen (2016), "WVC 2016: The Laser Craze", The SkeptVet.
- ^ Ingold N (2015). Lichtduschen Geschichte einer Gesundheitstechnik, 1890–1975 (in German). Chronos Verlag. pp. 40–49. hdl: 20.500.12657/31817. ISBN 978-3-0340-1276-8.
- ^ "The Nobel Prize in Physiology or Medicine 1903". Nobelprize.org. Nobel Media AB. 2016-11-01. Archived from the original on 2016-10-22. Retrieved 2016-11-01.
- ^ "Engines of our Ingenuity No. 1769: NIELS FINSEN". Retrieved 2014-04-05.
- ^ a b c Perera J (19 March 1987). "The 'healing laser' comes into the limelight'". New Scientist.
- ^ "Celebrating the 100th birthday of Professor Endre Mester". Laser World. Swedish Laser-Medical Society. April 18, 2004. Archived from the original on March 3, 2016.
- ^ "What Is Red Light Therapy?". WebMD. Retrieved 2021-02-11.
- ^ American Cancer Society. Cold Laser Therapy Page archived April 24, 2015
- ^ Lapchak PA (December 2010). "Taking a light approach to treating acute ischemic stroke patients: transcranial near-infrared laser therapy translational science". Annals of Medicine. 42 (8): 576–86. doi: 10.3109/07853890.2010.532811. PMC 3059546. PMID 21039081.
- ^ "District Court Grants Permanent Injunction Against Device Maker". Policy & Medicine. 5 May 2018. Retrieved 2021-02-11.
- ^ Hein A (2018-04-24). "'QLaser' TV infomercial doc gets 12 years in prison for selling scam device". Fox News. Retrieved 2021-02-11.
- ^ "A Skeptical Look at Low Level Laser Therapy | Quackwatch". 26 April 2018. Retrieved 2020-02-28.
- ^ Blue Cross and Blue Shield of Kansas City (Blue KC). "Low-Level Laser Therapy" (PDF). Policy No. 2.01.56. Retrieved 2 February 2019. (Policy reviewed each June; if link is dead try replacing "06-18" with a more recent year.)
- ^ "Infrared therapy". Aetna clinical policy bulletin 0363, reviewed June 17, 2020. Aetna has additional information in its "Clinical Policy Bulletin on Cold Laser and High-Power Laser Therapies".
- ^ "Decision memo for infrared therapy devices" (CAG00291N). Center for Medicare & Medicaid Services, Oct 24, 2006.
- ^ "Cigna Medical Coverage Policy- Therapy Services Low-Level Laser and High-Power Laser Therapy" (PDF). Cigna Medical Coverage Policy. Retrieved 2021-02-11.
- ^ Nampo FK, Cavalheri V, Ramos Sd, Camargo EA (2016-01-01). "Effect of low-level phototherapy on delayed onset muscle soreness: a systematic review and meta-analysis". Lasers in Medical Science. 31 (1): 165–177. doi: 10.1007/s10103-015-1832-4. ISSN 1435-604X. PMID 26563953. S2CID 21912028.
- ^ Ferraresi C, Hamblin MR, Parizotto NA (1 November 2012). "Low-level laser (light) therapy (LLLT) on muscle tissue: performance, fatigue and repair benefited by the power of light". Photonics & Lasers in Medicine. 1 (4): 267–286. doi: 10.1515/plm-2012-0032. PMC 3635110. PMID 23626925.
- ^ Yousefi-Nooraie R, Schonstein E, Heidari K, Rashidian A, Pennick V, Akbari-Kamrani M, Irani S, Shakiba B, Mortaz Hejri S, Mortaz Hejri SO, Jonaidi A (2008). Yousefi-Nooraie R (ed.). "Low level laser therapy for nonspecific low-back pain" (PDF). Cochrane Database of Systematic Reviews. 2011 (2): CD005107. doi: 10.1002/14651858.CD005107.pub4. PMC 9044120. PMID 18425909.
- ^ Middelkoop M, Rubinstein SM, Kuijpers T, Verhagen AP, Ostelo R, Koes BW, Van Tulder MW (2010). "A systematic review on the effectiveness of physical and rehabilitation interventions for chronic non-specific low back pain". European Spine Journal. 20 (1): 19–39. doi: 10.1007/s00586-010-1518-3. PMC 3036018. PMID 20640863.
-
^ Kadhim-Saleh A, Maganti H, Ghert M, Singh S, Farrokhyar F (2013-10-01). "Is low-level laser therapy in relieving neck pain effective? Systematic review and meta-analysis". Rheumatology International. 33 (10): 2493–2501.
doi:
10.1007/s00296-013-2742-z.
ISSN
1437-160X.
PMID
23579335.
S2CID
7057247.
his systematic review provides inconclusive evidence because of significant between-study heterogeneity and potential risk of bias.
- ^ Naterstad IF, Joensen J, Bjordal JM, Couppé C, Lopes-Martins RA, Stausholm MB (2022-09-28). "Efficacy of low-level laser therapy in patients with lower extremity tendinopathy or plantar fasciitis: systematic review and meta-analysis of randomised controlled trials". BMJ Open. 12 (9): e059479. doi: 10.1136/bmjopen-2021-059479. ISSN 2044-6055. PMC 9528593. PMID 36171024.
- ^ Naterstad IF, Joensen J, Bjordal JM, Couppé C, Lopes-Martins RA, Stausholm MB (2022-09-28). "Efficacy of low-level laser therapy in patients with lower extremity tendinopathy or plantar fasciitis: systematic review and meta-analysis of randomised controlled trials". BMJ Open. 12 (9): e059479. doi: 10.1136/bmjopen-2021-059479. ISSN 2044-6055. PMC 9528593. PMID 36171024.
- ^ Lourinho I, Sousa T, Jardim R, Pinto AC, Iosimuta N (2023). "Effects of low-level laser therapy in adults with rheumatoid arthritis: A systematic review and meta-analysis of controlled trials". PLOS ONE. 18 (9): e0291345. Bibcode: 2023PLoSO..1891345L. doi: 10.1371/journal.pone.0291345. ISSN 1932-6203. PMC 10490856. PMID 37683021.
- ^ Lourinho I, Sousa T, Jardim R, Pinto AC, Iosimuta N (2023). "Effects of low-level laser therapy in adults with rheumatoid arthritis: A systematic review and meta-analysis of controlled trials". PLOS ONE. 18 (9): e0291345. Bibcode: 2023PLoSO..1891345L. doi: 10.1371/journal.pone.0291345. ISSN 1932-6203. PMC 10490856. PMID 37683021.
- ^ Lourinho I, Sousa T, Jardim R, Pinto AC, Iosimuta N (2023). "Effects of low-level laser therapy in adults with rheumatoid arthritis: A systematic review and meta-analysis of controlled trials". PLOS ONE. 18 (9): e0291345. Bibcode: 2023PLoSO..1891345L. doi: 10.1371/journal.pone.0291345. ISSN 1932-6203. PMC 10490856. PMID 37683021.
- ^ Chen J, Huang Z, Ge M, Gao M (2015-04-01). "Efficacy of low-level laser therapy in the treatment of TMDs: a meta-analysis of 14 randomised controlled trials". Journal of Oral Rehabilitation. 42 (4): 291–299. doi: 10.1111/joor.12258. ISSN 1365-2842. PMID 25491183.
- ^ Haslerud S, Magnussen LH, Joensen J, Lopes-Martins RA, Bjordal JM (2015-06-01). "The efficacy of low-level laser therapy for shoulder tendinopathy: a systematic review and meta-analysis of randomized controlled trials". Physiotherapy Research International. 20 (2): 108–125. doi: 10.1002/pri.1606. hdl: 1956/17899. ISSN 1471-2865. PMID 25450903.
- ^ Page MJ, Green S, Kramer S, Johnston RV, McBain B, Buchbinder R (Oct 1, 2014). "Electrotherapy modalities for adhesive capsulitis (frozen shoulder)". The Cochrane Database of Systematic Reviews. 2014 (10): CD011324. doi: 10.1002/14651858.CD011324. PMC 10898218. PMID 25271097. S2CID 32666794.
- ^ Karlsson MR, Diogo Löfgren CI, Jansson HM (2008). "The Effect of Laser Therapy as an Adjunct to Non-Surgical Periodontal Treatment in Subjects with Chronic Periodontitis: A Systematic Review". Journal of Periodontology. 79 (11): 2021–2028. doi: 10.1902/jop.2008.080197. PMID 18980508.
- ^ Sgolastra F, Petrucci A, Severino M, Gatto R, Monaco A (2013-06-01). "Lasers for the treatment of dentin hypersensitivity: a meta-analysis". Journal of Dental Research. 92 (6): 492–499. doi: 10.1177/0022034513487212. ISSN 1544-0591. PMID 23609160. S2CID 25494366.
- ^ Eslamian L, Borzabadi-Farahani A, Hassanzadeh-Azhiri A, Badiee M, Fekrazad R (2013-01-20). "The effect of 810-nm low-level laser therapy on pain caused by orthodontic elastomeric separators". Lasers in Medical Science. 29 (2): 559–564. doi: 10.1007/s10103-012-1258-1. PMID 23334785. S2CID 25416518.
- ^ Ren C, McGrath C, Yang Y (2015-09-01). "The effectiveness of low-level diode laser therapy on orthodontic pain management: a systematic review and meta-analysis". Lasers in Medical Science. 30 (7): 1881–1893. doi: 10.1007/s10103-015-1743-4. ISSN 1435-604X. PMC 4562996. PMID 25800534.
- ^ He WL, Yu FY, Li CJ, Pan J, Zhuang R, Duan PJ (2015-08-01). "A systematic review and meta-analysis on the efficacy of low-level laser therapy in the management of complication after mandibular third molar surgery". Lasers in Medical Science. 30 (6): 1779–1788. doi: 10.1007/s10103-014-1634-0. ISSN 1435-604X. PMID 25098769. S2CID 22627779.
-
^ Rangwala S, Rashid RM (Feb 2012). "Alopecia: a review of laser and light therapies". Dermatology Online Journal. 18 (2): 3.
doi:
10.5070/D31JT041T2.
ISSN
1087-2108.
PMID
22398224.
Since then, a number of studies have suggested the use of lasers as an effective way to treat alopecia, particularly androgenetic alopecia and alopecia areata, but there is still a paucity of independent, peer-reviewed blinded clinical trials.
- ^ Avci P, Gupta GK, Clark J, Wikonkal N, Hamblin MR (February 2014). "Low-Level Laser (Light) Therapy (LLLT) for Treatment of Hair Loss". Lasers in Surgery and Medicine. 46 (2): 144–151. doi: 10.1002/lsm.22170. ISSN 0196-8092. PMC 3944668. PMID 23970445.
- ^ Gupta AK, Daigle D (April 2014). "The use of low-level light therapy in the treatment of androgenetic alopecia and female pattern hair loss". The Journal of Dermatological Treatment. 25 (2): 162–3. doi: 10.3109/09546634.2013.832134. PMID 23924031. S2CID 13565213.
- ^ Zarei M, Wikramanayake TC, Falto-Aizpurua L, Schachner LA, Jimenez JJ (2015-12-21). "Low level laser therapy and hair regrowth: an evidence-based review". Lasers in Medical Science. 31 (2): 363–71. doi: 10.1007/s10103-015-1818-2. ISSN 1435-604X. PMID 26690359. S2CID 22028662.
- ^ Darwin E, Heyes A, Hirt PA, Wikramanayake T, Jimenez JJ (2018). "Low-level laser therapy for the treatment of androgenic alopecia: a review". Lasers in Medical Science. 33 (2): 425–434. doi: 10.1007/s10103-017-2385-5. PMID 29270707. S2CID 23783876.
- ^ Liu KH, Liu D, Chen YT, Chin SY (2019-01-31). "Comparative effectiveness of low-level laser therapy for adult androgenic alopecia: a system review and meta-analysis of randomized controlled trials". Lasers in Medical Science. 34 (6). Springer Science and Business Media LLC: 1063–1069. doi: 10.1007/s10103-019-02723-6. ISSN 0268-8921. PMID 30706177. S2CID 59524423.
- ^ Gupta AK, Carviel JL (2019-11-20). "Meta-analysis of photobiomodulation for the treatment of androgenetic alopecia". Journal of Dermatological Treatment. 32 (6). Informa UK Limited: 643–647. doi: 10.1080/09546634.2019.1688755. ISSN 0954-6634. PMID 31746251. S2CID 208185306.
- ^ Zhang Y, Su J, Ma K, Fu X, Zhang C (2022-04-25). "Photobiomodulation Therapy With Different Wavebands for Hair Loss: A Systematic Review and Meta-Analysis". Dermatologic Surgery. 48 (7). Ovid Technologies (Wolters Kluwer Health): 737–740. doi: 10.1097/dss.0000000000003472. ISSN 1076-0512. PMID 35510860. S2CID 248526019.
- ^ Gupta AK, Bamimore MA, Foley KA (2020-04-13). "Efficacy of non-surgical treatments for androgenetic alopecia in men and women: a systematic review with network meta-analyses, and an assessment of evidence quality". Journal of Dermatological Treatment. 33 (1). Informa UK Limited: 62–72. doi: 10.1080/09546634.2020.1749547. ISSN 0954-6634. PMID 32250713. S2CID 215405183.
- ^ Darwin E, Heyes A, Hirt PA, Wikramanayake TC, Jimenez JJ (2017-12-21). "Low-level laser therapy for the treatment of androgenic alopecia: a review". Lasers in Medical Science. 33 (2). Springer Science and Business Media LLC: 425–434. doi: 10.1007/s10103-017-2385-5. ISSN 0268-8921. PMID 29270707. S2CID 23783876.
- ^ S L, P V, Y P, P J, T T (2021). "A Systematic Review and Meta-analysis of Randomized Controlled Trials of United States Food and Drug Administration-Approved, Home-use, Low-Level Light/Laser Therapy Devices for Pattern Hair Loss: Device Design and Technology". The Journal of Clinical and Aesthetic Dermatology. 14 (11): E64–E75. ISSN 1941-2789. PMC 8675345. PMID 34980962.
- ^ Smoot B, Chiavola-Larson L, Lee J, Manibusan H, Allen DD (2015-06-01). "Effect of low-level laser therapy on pain and swelling in women with breast cancer-related lymphedema: a systematic review and meta-analysis". Journal of Cancer Survivorship: Research and Practice. 9 (2): 287–304. doi: 10.1007/s11764-014-0411-1. ISSN 1932-2267. PMID 25432632. S2CID 27555240.
- ^ Smoot B, Chiavola-Larson L, Lee J, Manibusan H, Allen DD (2015). "Effect of low-level laser therapy on pain and swelling in women with breast cancer-related lymphedema: a systematic review and meta-analysis". Journal of Cancer Survivorship. 9 (2): 287–304. doi: 10.1007/s11764-014-0411-1. ISSN 1932-2259. PMID 25432632. S2CID 27555240.
- ^ Borzabadi-Farahani A (2016-07-22). "Effect of low-level laser irradiation on proliferation of human dental mesenchymal stem cells; a systemic review". Journal of Photochemistry and Photobiology B: Biology. 162: 577–582. doi: 10.1016/j.jphotobiol.2016.07.022. PMID 27475781.
- ^ a b Bouzari N, Elsaie ML, Nouri K (2012). "Laser and Light for Wound Healing Stimulation". In Nouri K (ed.). Lasers in Dermatology and Medicine. Springer London. pp. 267–275. doi: 10.1007/978-0-85729-281-0_20. ISBN 978-0-85729-281-0.
- ^ Posten W, Wrone DA, Dover JS, Arndt KA, Silapunt S, Alam M (2005). "Low-level laser therapy for wound healing: mechanism and efficacy". Dermatol Surg. 31 (3): 334–340. doi: 10.1111/j.1524-4725.2005.31086. PMID 15841638. S2CID 129167.